Mi Nguyen
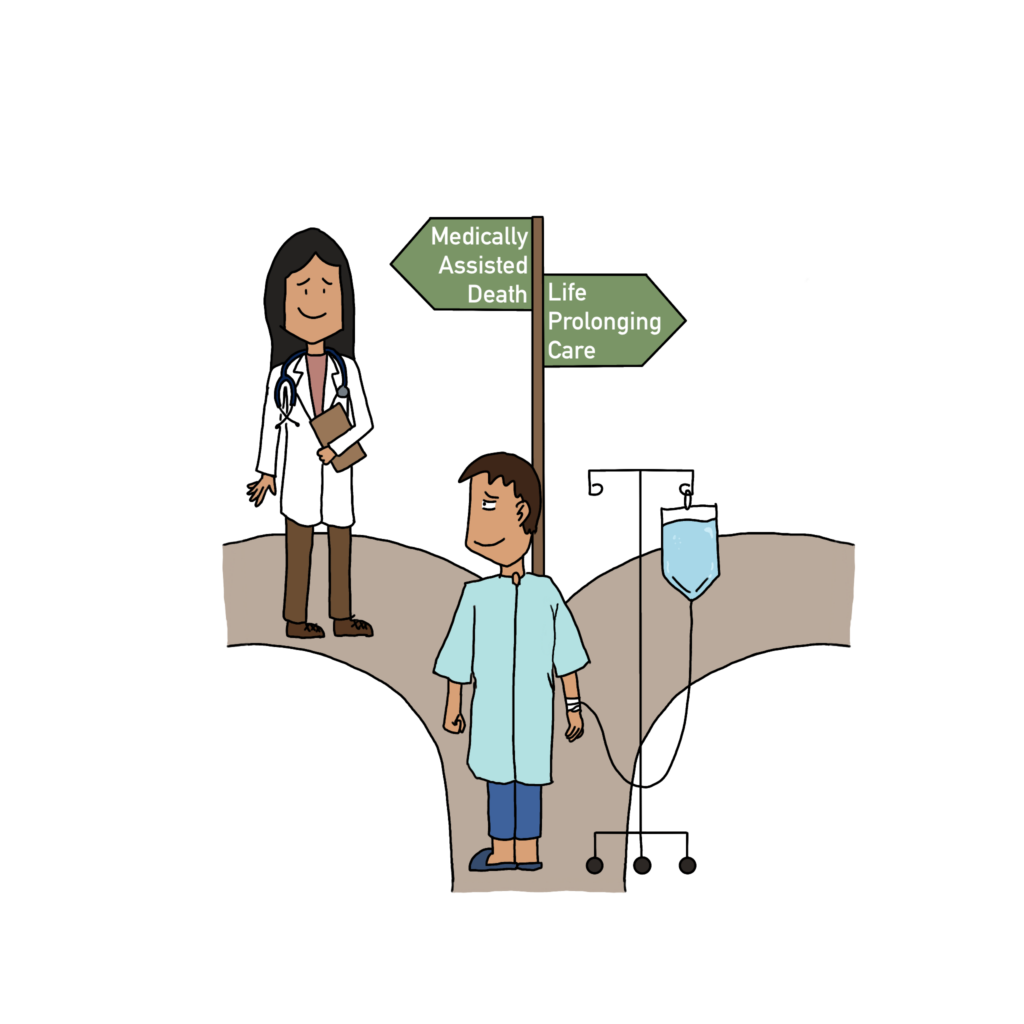
In 1997, Oregon became the first U.S. state to legalize physician-assisted death under the Death with Dignity Act. Over the last two decades, the law inspired similar legislation across the globe. In the U.S., physician-assisted death is now legal in 13 states — California, Washington, Colorado, Hawaii, Maine, New Jersey, New Mexico, Vermont, Montana, Illinois, Delaware, New York and Oregon — and the District of Columbia. This policy has extended to countries like Canada, the Netherlands, Switzerland and Colombia, and ranges in specifics — in Switzerland, physician assisted death can be performed by non-physicians. The passage of physician-assisted death laws marked a shift in medical ethics and public policy, putting patient autonomy at the forefront of care.
Physician-assisted death can be described as a physician indirectly aiding in a patient’s death, whether than means providing them with the means and knowledge of how to end their life — often through doses of drugs — or honoring their wish to stop or refuse treatment to prolong their life.
For patients who are terminally ill, life can become a prolonged sense of dying, defined by pain, dependence and a loss their of control.
“If [the patient] has six months to live, it is [already like] death,” said junior Ronon Lohr.
By giving patients the legal right to choose when and how to end their life, physician-assisted death lets them make a decision without being at the mercy of a debilitating disease.
Passed in California, the End of Life Option Act allows for physician-assisted death so long as certain requirements are fulfilled: the patient must be an adult, able to make their own informed decisions and have a prognosis of six months or less to request medication to peacefully end their lives. The law is deliberate and heavily regulated. Patients must make multiple requests, receive confirmation from two physicians and show mental competence. These safeguards exist because the decision is serious. But just because a choice holds gravity does not make it immoral.
In fact, denying the option of physician-assisted death is what crosses a line.
“It allows someone to die with control and dignity,” said junior Macklin Berg. “I don’t think it devalues life at all. Devaluing life would be if they didn’t choose to die and people around them were choosing for them.”
Denying a terminally ill person the right to die peacefully and take control of their death does not protect life, and it is a self-centered way to exercise control over the lives and personhood of others.
It is important to clarify the distinction between physician-assisted death and suicide, which is defined as the act of intentionally taking one’s own life. Suicide occurs in circumstances in which life might otherwise continue, and is often motivated by mental illness or isolation. Physician-assisted death, by contrast, is sought by patients whose lives are, by medical standards, coming to an end, and whose desire is not to escape life itself but to exercise control over the manner in which it concludes.
“Suicide is … choos[ing] to die in face of living,” Berg said. “[Physician-assisted death] is … choosing to die in the face of death.”
Life should not be defined as a mere biological function, but by the presence of a meaningful existence. It is extremely important to make the distinction.
Insisting that a person must remain alive at all costs, even when their mobility and autonomy have been diminished, steals their authority over their individual judgement.